Chronic mucocutaneous candidiasis: a spectrum of genetic disorders
Abstract
Introduction
Candida infection in healthy and immunocompromised individuals
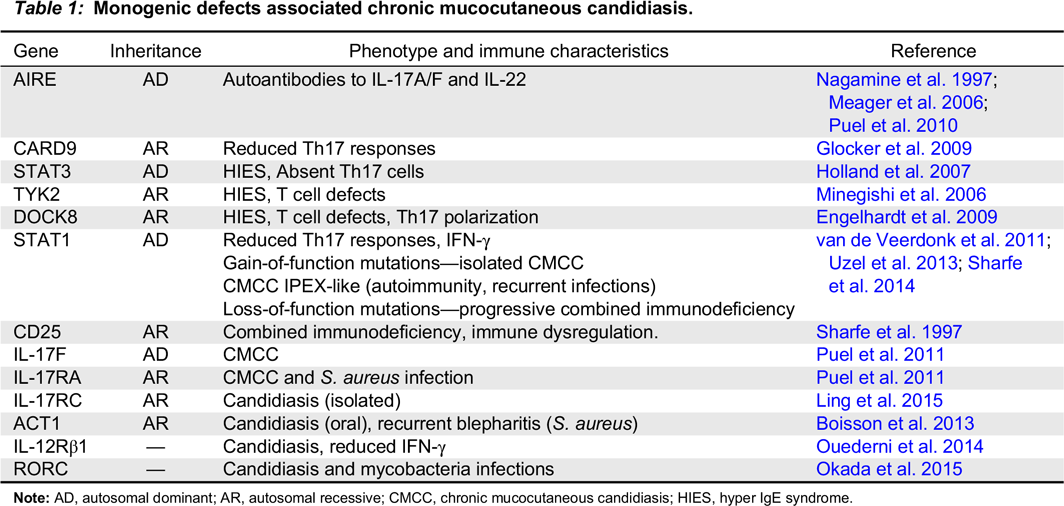
Note: AD, autosomal dominant; AR, autosomal recessive; CMCC, chronic mucocutaneous candidiasis; HIES, hyper IgE syndrome.
Detection of Candida by immune cells
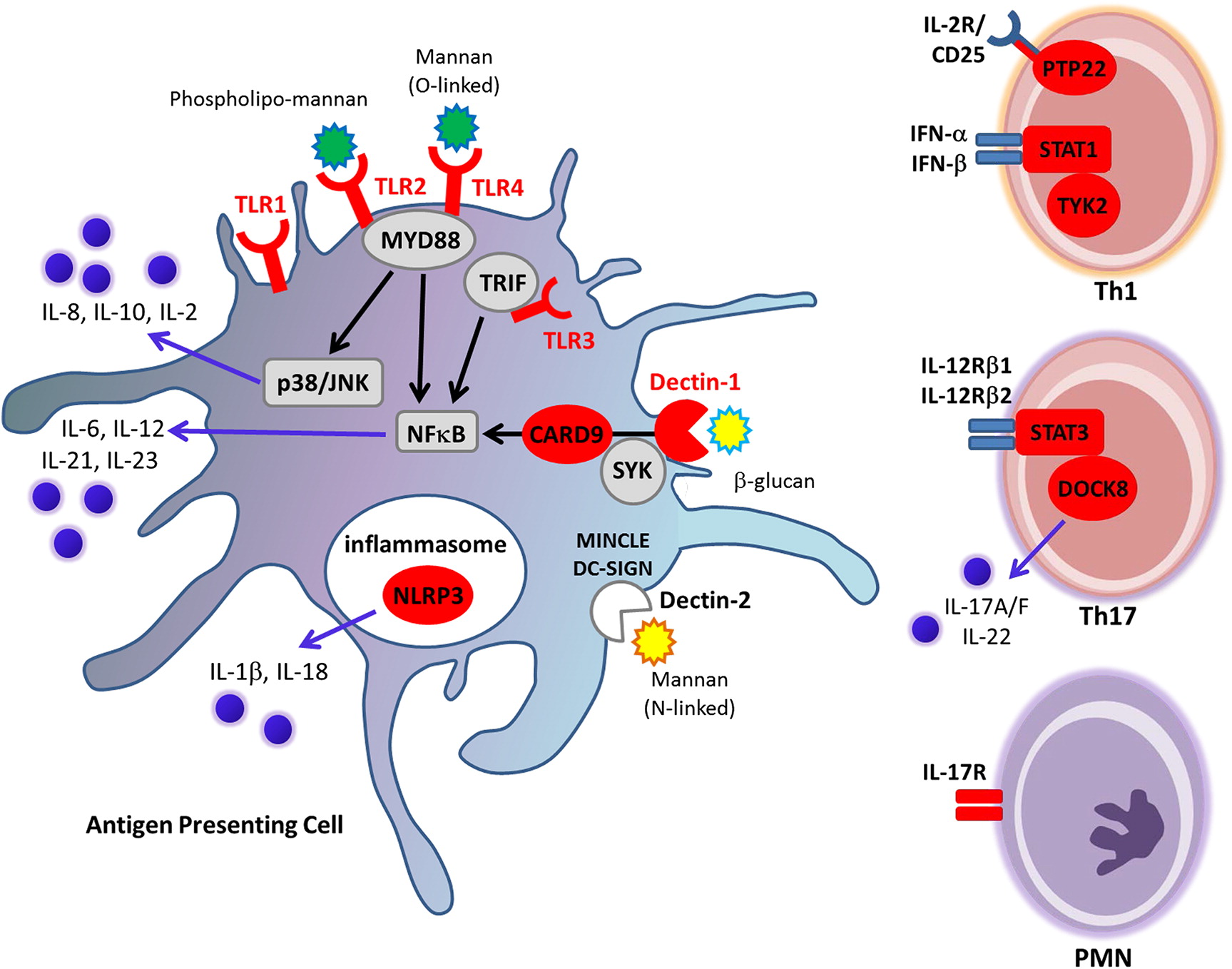
Monogenic defects causing CMCC
Autoimmune regulator (AIRE) deficiency
Signal transducer and activator of transcription-1 (STAT1) dysfunction
Caspase recruitment domain-containing protein 9 (CARD9) deficiency
Interleukin-17 pathway defects
Signal transducer and activator of transcription-3 (STAT3) dysfunction
Dedicator of cytokinesis 8 (DOCK8) deficiency
Tyrosine Kinase 2 (TYK2) deficiency
CD25 deficiency
Protein tyrosine phosphatase non-receptor type-22 (PTPN22) mutations
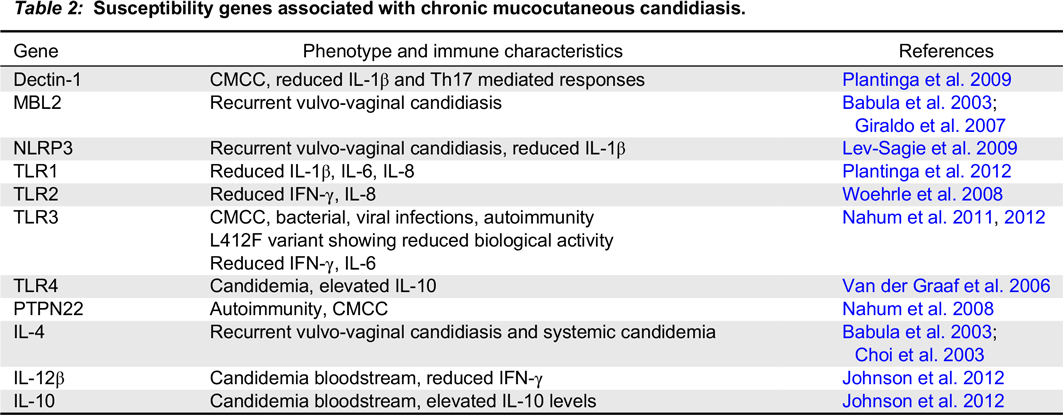
Susceptibility genes associated with CMCC
Concluding remarks
REFERENCES
Information & Authors
Information
Published In

History
Copyright
Authors
Metrics & Citations
Metrics
Other Metrics
Citations
Cite As
Export Citations
If you have the appropriate software installed, you can download article citation data to the citation manager of your choice. Simply select your manager software from the list below and click Download.
Cited by
View Options
View options
Login options
Check if you access through your login credentials or your institution to get full access on this article.


